Hey, this is me, your doctor. You died.
Let’s get this out of the way: there are a couple people in this auditorium who I probably killed.
I wasn’t trying to, of course, but we’ll get to that.
You were not the first people in my care who died, of course. Death comes with my job. People don’t come to the hospital because everything is going super great and they’re having a fun time. They’re sick, many are elderly, and many have been in the hospital seven times in the last six months.
But you are the ones who haunt me when I try to sleep at night.
Every culture has a different idea of what constitutes a good death. Some people want to die in battle. Some people want to die as martyrs. In our culture, we want to die from old age. We want to die in bed, in our sleep. If we can’t have that death, we want to die in a hospital bed with clean white sheets, surrounded by family and sympathetic doctors and nurses. We want them to mourn us and celebrate us as we pass into the dark.
In contrast, the ideas about what constitutes a bad death are a little more unified across cultures. A bad death is an unanticipated death or an excruciating death. We fear, worst of all, that we will die alone — and that no one will know what happened to us.
You died the worst kind of death, and for all of my training, all of my sophistication and artistry, I was powerless to stop it.
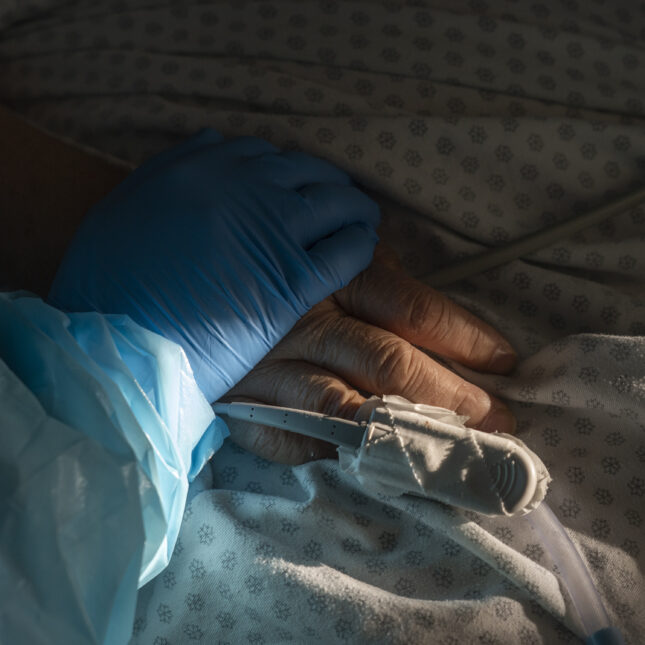
You died gasping.
When I talk about suffering to patients and their families, I contextualize it as “the four horsemen.” The four horsemen of suffering are pain, itch, nausea, and breathlessness. All four of these can become such an excruciating torment that they can they rob us of our wits, that they can cause people to beg for relief — but for the first three, for pain, itch and nausea, eventually, even if relief isn’t possible, people curl up, they withdraw into themselves, and they shut down.
But with breathlessness, we stay awake. We fight until our very last gasp.
Covid-19 causes acute respiratory distress syndrome, a form of pneumonia so severe I had only seen it two or three times. Then, in April 2020, every single bed in my hospital was full of Covid patients. Many had ARDS.
Those who don’t die from the pneumonia die from the blood clots, which can block the vessels of the lungs instantly, preventing gas exchange.
Worst of all, though: you died alone.
Because we didn’t have enough personal protective equipment, we often just left you alone with the sedation drips and the ventilator running when we knew you were dying. We had to go save other people, people who had only been on the vent a few days, people we thought might have made it.
Look at the two people sitting beside you.
One of those people, I abandoned to die alone.
One of those people is the person I abandoned them for. That’s the person I tried to save, who I tried to save desperately, who I gave more resources and time than calculating clinical logic should have allowed.
Maybe one of those people is one where I had an impossible choice — a choice between bad and worse — and I still managed to choose wrong.
One of you was in kidney failure due to profound dehydration. When I gave you IV fluids to try to preserve your kidney function, even though it was the smallest order for fluids I’d written in my career, it was still enough to flood your damaged lungs. After that, all I could do was give you a little morphine to take the edge off while you drowned.
One of you got so confused that you pulled off your mask. You pulled it so hard it broke something behind the wall. I knew how to get the mask back on, I knew how to troubleshoot the BiPAP machine, but by the time I realized that the problem was in the wall, by the time I yelled for someone to get a portable oxygen tank…. You couldn’t speak, but you were looking into my eyes. You knew I was the doctor who had helped you feel better every other time your breathing got bad. Why wasn’t I helping you this time? You died before they found the oxygen tank.
There are lots of other stories, of course, but we don’t have eternity — well, I don’t, at least. I’m sorry, I’m really sorry. I hope you don’t think I didn’t care, because I always did. I wish at this point that I was one of those people that could hit a button and turn off my “give a fuck” switch but that’s not possible for me. So this little talk, this goodbye, is the next best thing.
You know, looking out at you now, I feel a little peace. I see how serene you are. I see quite a few of you as I never got to see you in life: together again, holding hands. Christ, though — it was hard, it was so hard, to explain to your kids that they were going to lose both Mom and Dad at the same time.
After the third or fourth time, I got better at that conversation. I made it easier on your children. But afterwards, every time, I would have to find a quiet place, and just sob, imagining if it was my Mom and Dad who had to die alone together, in separate ICU beds one room apart.
Your families miss you so much.
They’d plead with me. That’s common, actually. No matter how many times I explain that I’m not in control, that the disease is in control, it’s much easier to pretend that someone has the power to fix it.
But the tools in the ICU, at best, are just a pause button.
I can hit pause.
I can’t rewind.
There are so many of you, I admit, that some of your faces now seem unfamiliar to me. Of all the guilt I carry with me, that’s the worst.
That I lost you once — that’s bad enough.
Then lost you again, when I fucking forgot.
I can already see you looking around the auditorium and then looking back at me like I’m losing my mind. That there are hundreds of you, that I couldn’t have possibly kept all that inside my head without going really and truly insane.
I know our time is almost up.
I can’t pretend this was easy, but it was good. It was good to see you all again. I will say goodbye the way I always said goodbye to your families: it was my honor and privilege to care for you.
That’s how you died.
Now, maybe, I’ll be able to say goodbye for good, and finally get some sleep.